Analysis: Countering misinformation, conspiracy theories causing booster shot hesitancy

KUALA LUMPUR: Nine months after the implementation of the National Covid-19 Immunisation Programme and with over 25 million of Malaysia’s population fully vaccinated, vaccine hesitancy is rearing its ugly head again.
But this time, it is over getting the Pfizer or AstraZeneca vaccine as a third shot, especially among Sinovac vaccine recipients.
In a pandemic that has spanned two years with many twists and turns – from mask usage to the emergence of the Alpha, Beta, and Delta variants to vaccine dosage – health guidance and decisions have been rapid and, to a layperson, ever-changing. Adding a booster shot of a different brand to the current vaccination strategy may be a bridge too far for a populace struggling to adapt.
Commenting on a news story on heterologous shots, a Facebook user from Kedah Tan Saw Choo said, “Why should I take Pfizer as my booster to clear up (your) stock. I (am) waiting for my Sinovac booster (and) not mix (and) match.”
Health Minister Khairy Jamaluddin recently tweeted that about 40 per cent of people are not showing up for their booster shot. He warned that if booster take-up is low, especially among the elderly and those with comorbidities, “hospitalisation numbers will go up”.
“This is for sure. If you get an appointment, take the booster,” he said.
Malaysia began administering Pfizer booster shots to front-liners, the elderly, and people with comorbidities last month as immunity began to wane and breakthrough cases started rising. Pfizer and AstraZeneca vaccine recipients are recommended to receive their booster six months after their last dose and Sinovac vaccine recipients three to six months after their last dose.
Although all three vaccines, as of Nov 17, received conditional approval to be administered as a booster shot in Malaysia, health authorities have recommended that Sinovac recipients get Pfizer or AstraZeneca as their third dose instead of Sinovac, unless they have allergy issues. This is called the heterologous vaccination regimen where one of the doses administered is a different type of vaccine.
Researchers in the United States, Chile, and elsewhere have found that using one of the messenger ribonucleic acid (mRNA) vaccines, that is, Moderna or Pfizer, or the viral vector AstraZeneca vaccine as a booster shot provided the best protection against Covid-19 in the long run.
Convincing people that it is safe to mix vaccine types is another matter, however. While the science is there to show heterologous shots work and are safe, many apparently consider vaccines like laundry: the red shirt should not be mixed with the white one.
Doctors in Johor and Sarawak have reported that a sizeable chunk of their patients who received Sinovac are refusing the Pfizer booster shot.
A cursory search on social media on Malaysians’ thoughts of mixing vaccines found many are unhappy about having to get the Pfizer vaccine as their booster shot. Most are afraid of the long-term side effects from mixing vaccines, as well as receiving the mRNA vaccine, a new technology. A few accused the government of falling for Western propaganda against China or trying to finish leftover Pfizer stock.
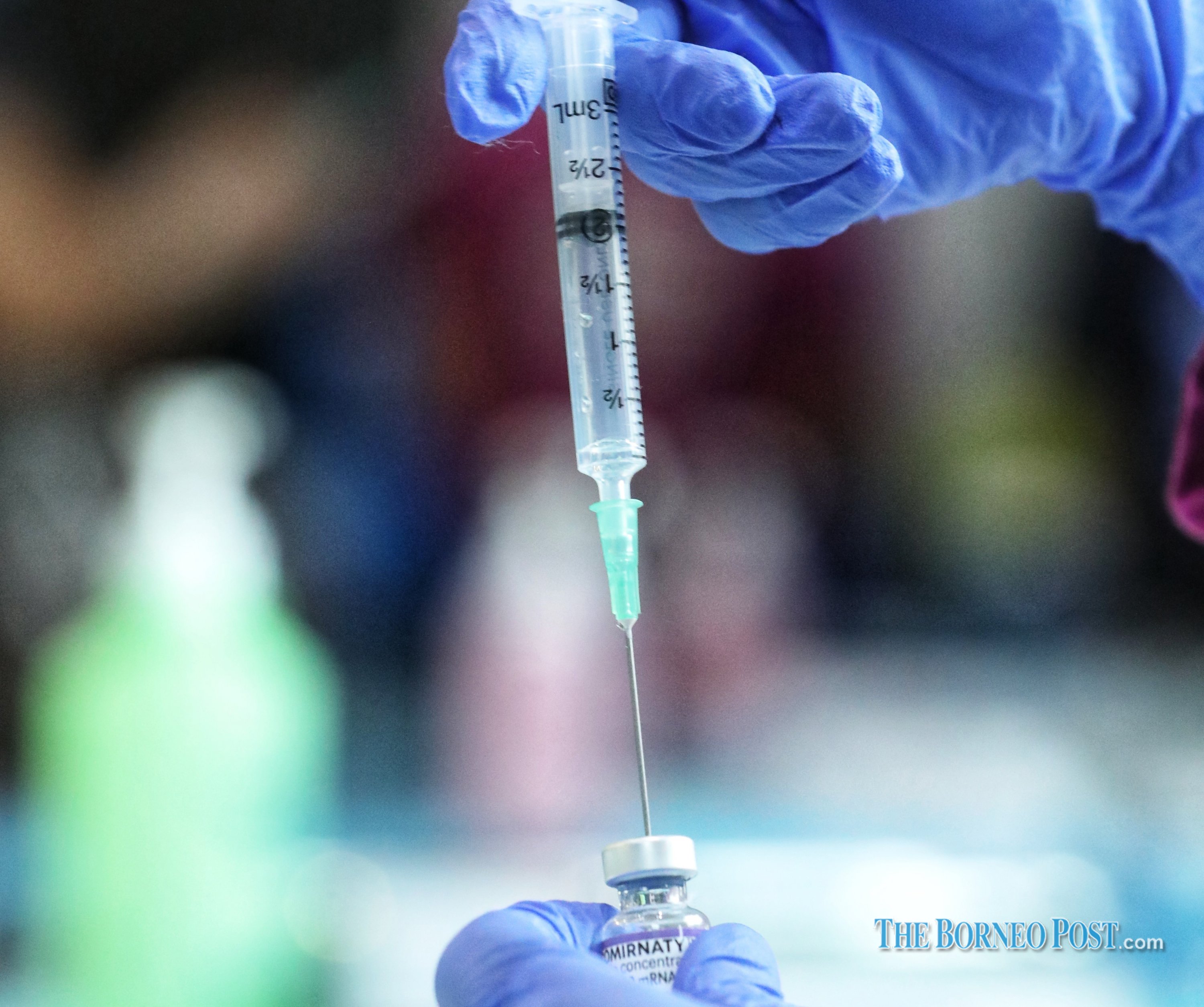
A health worker prepares a dose of the Pfizer Covid-19 vaccine. — Photo by Chimon Upon
Mixing works
While the mRNA may be a new vaccine technology, mixing vaccine types is not new.
Virologist Dr Vinod Balasubramaniam told Bernama Johnson and Johnson has done it before with their Ebola vaccine, which has a two-dose regimen. One is a monovalent vaccine while the other is an attenuated (weakened) vaccine of a pox virus.
Furthermore, he said studies in Europe, South America, and elsewhere on heterologous Covid-19 vaccinations have continued showing how effective mixing and matching vaccines can be.
“With vaccination, our bodies have a picture (of the virus). Now, mixing two different types of vaccines means we are showing two different angles of the picture so your memory gains that particular photo of the pathogen. It becomes better, rather than using the same angle. That’s what mixing and matching does,” he said.
While Europe has been using a mix of AstraZeneca and Pfizer vaccines, in some countries – due to the shortage of supply since May – actual studies testing the efficacy of Sinovac and boosted with AstraZeneca, Pfizer, or Sinovac have come out with their findings.
A study conducted by the Chilean Ministry of Health and presented to the World Health Organisation on Oct 25 found that Sinovac recipients who got either AstraZeneca or Pfizer as a booster shot received 91 and 93 per cent protection respectively against infection, and 97 and 91 per cent protection against hospitalisation.
Sinovac recipients who received a third dose of Sinovac were only protected against infection 71 per cent of the time and 85 per cent against hospitalisation.
Explaining how the Covid-19 vaccine works, Associate Prof Dr Nazlina Ibrahim, a virologist with Universiti Kebangsaan Malaysia, said the immune system has three parts: the macrophage, T-cells, and B-cells. The macrophage eats an intruder or dead cells. It leaves behind parts of the invading germs or virus called antigen, which the body identifies as dangerous and tells T-cells and B-cells to produce antibodies to kill them. T-cells attack infected cells while B-cells attack the leftover antigen.
In an unvaccinated person, when the body encounters a virus or germ for the first time, it takes a few days for it to figure out how to attack the intruder and produce the tools to get rid of the infection. Assuming the person survives, the body then remembers how to fight the intruder for a time.
Vaccination simulates that infection, teaching the immune system to recognise the specific virus – in Covid-19’s case, it is the spike protein the virus uses to latch onto healthy cells.
Dr Nazlina said the Chilean study showed the Sinovac vaccine only produced antibodies by B cells, not T-cells, while a shot of Pfizer provided a robust T-cell response to kill the infected cells.
“When we combine the two vaccines, we get a better type of protection in terms of immunity,” she said.
As for possible long-term health problems, both she and Dr Vinod say vaccines do not work like that as they are not drugs, which can cause long-term health problems.
According to the US Centers for Disease Control (CDC), the chances that vaccines, including Covid-19 vaccines, cause long-term side effects are extremely low. Side effects or adverse reactions usually occur within six months of receiving a vaccine dose.
More than 3.22 billion people worldwide have received the full doses of the Covid-19 vaccines with very few serious side effects or adverse reactions recorded.
“The main long-term side effect of vaccines is survival, which is why we are alive now,” added Dr Vinod.
A health worker prepares a dose of the Pfizer Covid-19 vaccine. — Bernama photo
Getting the message across
However, as safe and effective as mixing and matching some Covid-19 vaccines are, relaying information on a complicated subject in an easily understandable way is not simple.
Many of the social media posts from Sinovac recipients who refuse to get the Pfizer booster shot were rife with misinformation and conspiracy theories. Peppered among these comments are pleas from other Malaysians, asking them to get their booster shot so cases would not rise and lead to another lockdown.
Communications expert Abdul Hamid Saifuddin said public service messages dealing with difficult subjects should be broken down into easy, everyday language to be effective.
“We have to break it down for them. We have to spell it out bit by bit. It’s taxing … but again, ultimately … people will understand, get them curious and most definitely they want to do something about it,” he said.
Hamid, who is also a lecturer in public relations at Universiti Teknologi Mara, said public health officials rely on too much jargon when trying to spread awareness, adding consistent and daily messaging would help increase awareness among the masses.
He also suggested that health authorities and interested parties use popular modern communication methods, such as memes and short TikTok videos, to explain the benefits of heterologous boosters to the “aunties and uncles on WhatsApp”.
However, both he and Dr Vinod think the government should not be the main spokesperson for this, as some Malaysians have grown sceptical of or blame health authorities, be it rightly or wrongly, for the ongoing pandemic.
Dr Vinod, who is attached to Monash University-Malaysia, said general practitioners and trusted family physicians, instead, should spearhead the effort to educate their patients on the benefits of mixing and matching the vaccines.
“Counselling from doctors will make a huge difference. (People) won’t listen to us but to a certain extent, they will listen to their doctors,” he said.
Clinics in the public and private sectors are responsible for vaccinations and are providing booster shots now. There are plans to reopen the vaccination centres to help with this effort. Walk-ins will soon be allowed with the list of sites to be announced on Nov 22.
Dr Nazlina, however, said when the message is delivered, people need to trust the science and realise the best way to protect themselves and their community is to get all the shots.
“Vaccination is … for you to have a barrier; it’s having something to shield yourself when the time comes. Prevention is better than cure,” she said. — Bernama